Physical therapists (PTs) are movement experts who understand all the individual components of movement, such as which joints move and what muscles work during any phase of any activity, e.g., walking, running, lifting, etc.
When you take a step, PTs know the muscles that are working and how much mobility you need in every joint of your body to keep you upright and moving forward, from the top of your head down to your big toe. PTs know that when you look to the right, without moving your head, that the small neck muscles at the base of your skull fire to keep your head forward. Using that knowledge base, PTs use many approaches to treating people to overcome their pain and movement limitations.
As an independent PT, I do not have to rely on a cookie-cutter approach to therapy as I have the luxury of having ample time to create very individualized exercise and manual therapy programs for my patients.
The ‘Elevator Pitch’: Traditional vs Non-Traditional Physical Therapy
This past year I have been getting out to meet people at networking events. At a networking event I use an “elevator speech” to describe my business in less than 1 minute (the average amount of time it takes to ride the elevator with someone).
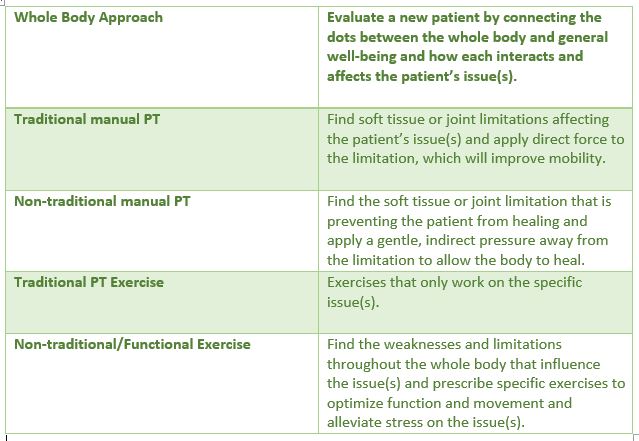
My elevator speech begins with “I use a whole body approach of traditional and non-traditional manual physical therapy and functional exercise to get people back to doing the things they love to do…..”
Whoa, but what does that really mean? Why do I use both traditional and non-traditional approaches?
Here is the long version of that elevator speech:
When I began my career as a PT, I started out doing traditional manual physical therapy, such as deep tissue work to free up soft tissue and joint limitations with good results, but a small percentage of people did not improve.
I began studying a non-traditional manual physical therapy approach called IMT, or Integrative Manual Therapy. After a couple of years of learning and using IMT, I realized IMT could help not only those people who did not get help from traditional physical therapy but also could help all my patients. So, I began to study IMT intensively to become a certified IMT practitioner. I did not, however, throw out the traditional approaches as they still worked when used appropriately.
IMT has taught me how to think of people as a whole being, physically, emotionally, and spiritually.
It has taught me to not just look at patients from a musculoskeletal perspective, but to look deeper, at the emotional and spiritual impact as well as the impact from all the other structures and systems in the body, such as the gastrointestinal (GI) system, the cardiovascular system, the renal system, etc., to see how those systems affect musculoskeletal pain and movement. A traditional PT will typically only look at the muscuoloskeletal structures such as bone, muscle, tendon or ligament.
For example, low back pain is often diagnosed as a muscle strain, which may be true, but the IMT approach views that muscle strain as the body’s intelligence taking over in order to protect the body from more serious damage, such as a herniated disc, tear in a blood vessel, or spinal cord injury.
Using IMT, I may treat other body systems/structures in order for the body to realize, “Oh, I don’t have to protect you anymore, so I can release the muscle strain.” Sometimes, a person with low back pain might have a GI diagnosis such as irritable bowel syndrome (IBS) or ulcerative colitis (UC), and since the GI system sits in front of your back, the GI system needs to be treated in order to alleviate the low back pain.
At The Manual Touch, after patients receive either traditional or non-traditional manual physical therapy, their bodies will have less tissue strain and improved joint mobility. They, then will need an exercise program to integrate their newfound mobility and optimize body function.
So, as a non-traditional complement to my manual skills, I became certified in Applied Functional Science (AFS). AFS is an approach to exercise that finds the patient’s weaknesses and limitations throughout the whole body that are influencing the issue(s), whether it be pain, mobility or function. I then prescribe specific exercises to re-educate the patient’s body to work together and alleviate stress influencing the issues(s). This approach allowed me to shift from prescribing a cookie-cutter approach of exercises for just the injured area, such as knee exercises for knee pain or shoulder exercises for shoulder pain, to prescribing an individualized exercise program to promote optimal body function.
Now, let’s take a look at the different approaches involved in physical therapy and explain them using real stories — Kathy and Carney.
Meet Kathy:
When Kathy came to see me, she had already been to physical therapy elsewhere that had provided minimal relief for her persistent upper back and neck pain and occasional low back pain.
Kathy had suffered a concussion the year prior and works full time at a desk job. Kathy said she likes to use a theracane on her upper back muscle spasm which temporarily relieves her pain.

A theracane is a device, like a back scratcher, that allows you to reach and apply pressure to those tough knots in your back by yourself similar to a traditional or direct manual physical therapy technique. She also did yoga and meditation.
After a full whole body evaluation we began treatment with the following explanation for Kathy’s chronic condition:
- When a condition lasts longer than 3-6 months it becomes chronic. People in chronic pain have a heightened nervous system, as their bodies are always in a state of fight or flight. I used non-traditional manual physical therapy to calm her nervous system. Read my blog post: Chronic pain and IMT
- A concussion needs the body to absorb the impact to the head down through the entire spine to the pelvis. It’s important to treat the bottom of the spine, the pelvis, and all the tissues within the spine and head to alleviate stress in the upper back. I used traditional and non-traditional manual physical therapy to treat the concussion aftermath.
- She had weakness in her core and her feet, which didn’t provide a base of support for her upper back, thus preventing her upper back from healing. By using a Whole Body Approach, Kathy was given functional exercises to promote the integration and strengthening of her feet and core.
- Kathy received education about better footwear, appropriate exercise classes, postural tips, and appropriate use of the theracane (minimizing use).
After 6 weeks of physical therapy, Kathy’s low back pain was gone, her upper back pain episodes had decreased to 1 time or so per month and she improved her strength and body awareness. Kathy now rarely uses her theracane.
Meet Carney:
Carney is a triathlete and marathon runner. He came to me with Achilles pain when walking or running.
Through his evaluation, I found he lacked the necessary mobility in his spine, hips, and ankles to run or walk optimally. In order to make up for this lack of mobility, his body found the movement elsewhere to complete the task of running or walking, ultimately creating an overuse syndrome of his Achilles.
Carney had to stop running for many months as he did a lot of functional exercises to improve his mobility, cross trained with bike, swim, aqua jog and elliptical, and he also received traditional and non-traditional manual physical therapy to promote healing. Carney’s mobility significantly improved and he went on to run the Chicago marathon this past year with no Achilles pain.
As you can see from these examples, the key to successful treatment is using a combination of approaches and knowing which phase of the healing process will respond to the best approach. At The Manual Touch Physical Therapy, we take great care in finding an individualized approach for each patient to facilitate the swiftest and safest route to recovery.

Is There a Solution for Lower Back Pain?
Are you struggling with lower back pain or sciatica? Is it keeping you from doing the activities you enjoy? If so, I’d like to invite you to our FREE workshop to learn the 3 main causes and how to heal naturally.
Click here to sign up for this free monthly workshop and learn how to get your life back.





I was in an accident, and I’m trying to recover from injuries. It makes sense that physical therapy would be important. Maybe I should see a professional to have them figure out what I need to have done! Having direct access would be nice, since then I would get treated a lot easier.
Hi Braden
sorry for the delay in replying, I didn’t realize there was a comment.
How are you doing? Feel free to give me a call to discuss your issues and we can figure out the best course of action for you
Denise